
Using AI for Veterinary Dental Radiograph Interpretation
Veterinary dental radiographs matter because a large share of meaningful oral disease sits where the eye cannot see it: below the gumline, around the roots, inside surrounding bone, and within structures that can look normal during a visual exam alone.
Professional guidance for veterinary dentistry has long emphasized that oral decisions should be based on both imaging and clinical findings, not on surface appearance alone.
That is exactly why AI for Veterinary Dental Radiograph Interpretation is getting so much attention. In busy practices, dental X-rays can be time-consuming to review tooth by tooth, especially when positioning is imperfect, findings are subtle, or the clinical team is balancing anesthesia time, charting, client communication, and treatment planning all at once.
Artificial intelligence does not replace the veterinarian, the dentist, or the radiologist. What it can do is act as an extra layer of pattern recognition, flagging abnormalities, organizing findings, and supporting more consistent review of every image in a case.
For readers trying to understand where this technology fits, the most helpful view is a practical one. AI in veterinary dentistry is neither magic nor menace.
It is a tool. When the images are diagnostic, the workflow is well designed, and the clinician stays firmly in charge, veterinary dental imaging AI can support faster reviews, stronger documentation, training for less experienced teams, and more confident communication with pet owners.
When image quality is poor, anatomy is unusual, or disease falls outside the tool’s training, caution is essential.
This article explains how AI veterinary dental radiograph interpretation works, what kinds of findings it may help identify, where it adds value, where it can mislead, and how to use it responsibly in real veterinary workflows.
If you want a broader background on technology adoption in clinics, resources on vet practice technology in workflow management, AI diagnostics in veterinary medicine, and cloud-based systems for veterinary practices provide useful context for how these tools fit into modern operations.
Why veterinary dental radiograph interpretation is so important
Veterinary dental X-ray interpretation is one of the most valuable parts of oral care because the most important disease is often hidden. A fractured crown may be obvious, but the true extent of root damage, bone loss, periapical change, retained roots, or tooth resorption may only become clear on radiographs.
That is why full-mouth imaging is widely treated as a core part of comprehensive dental assessment rather than an optional add-on.
Interpretation, however, is not simple. The clinician is not just asking, “Is there disease?” They are asking a series of more detailed questions: Is the image diagnostic? Is the tooth anatomy normal for this patient? Is there periodontal bone loss, furcation involvement, widened periodontal ligament space, root lysis, pulp exposure, ankylosis, or apical pathology? Are there changes that alter the treatment plan, the prognosis, or the urgency of care? That level of review requires both technical skill and repetition.
The challenge grows because every mouth is a little different. Skull shape, breed type, age, tooth overlap, prior extractions, crowding, rotation, and positioning errors can change what an image looks like.
Even a careful reader can lose time or confidence when reviewing dozens of teeth under procedural pressure. This is one reason AI-assisted veterinary radiology is appealing: it promises support at the exact point where careful, repetitive image review matters most.
What makes dental radiograph interpretation challenging in animal patients
Unlike many other imaging tasks, dental radiograph software for veterinarians must deal with very small structures, subtle contrast differences, and anatomy that can change dramatically from one patient to another.
A small amount of root lysis, early loss of lamina dura, or a faint periapical change can matter clinically, yet those findings may be easy to overlook when the image is slightly stretched, foreshortened, or overlapped.
Another challenge is that interpretation never happens in a vacuum. The person reading the image may also be monitoring workflow, thinking about anesthesia time, coordinating with a technician, updating a chart, and planning extractions.
That mental load increases the value of consistent review tools but also explains why false reassurance can be dangerous. A missed alert from AI is not the only risk; overtrusting a clean AI result can be just as problematic.
Veterinary patients also introduce variation that some human dental imaging systems never had to handle. Dogs and cats differ from one another, and within those groups there is substantial range in skull conformation, tooth spacing, tooth size, and common disease patterns.
Add age-related change, deciduous tooth retention, oral masses, advanced periodontal destruction, and prior dental work, and the image landscape becomes even more complex.
This is why experienced clinicians often describe veterinary dental X-ray interpretation as both technical and contextual. The image has to be read correctly, but it also has to be understood alongside probing, charting, mobility, oral exam findings, history, and planned treatment.
AI veterinary imaging diagnostics can help organize that process, but it must be built around the reality that radiographs are one part of a broader clinical decision.
Why consistency matters just as much as speed
Many discussions of AI veterinary dental radiograph interpretation focus on speed, and speed does matter. Shorter review times can support smoother anesthesia workflows, faster treatment decisions, and better team coordination. But consistency may be the bigger gain in day-to-day practice.
A consistent review process means every tooth gets attention, every image is assessed against a repeatable standard, and important findings are less likely to depend on who happens to be reading the film at that moment.
That is especially valuable in multi-doctor hospitals, general practices with varying levels of dental comfort, and teams that are still building confidence in diagnostic imaging in animal dentistry.
Consistency also improves communication. When the review is structured, the team can explain findings more clearly to clients, compare cases more easily over time, and document treatment rationale in a way that holds up later.
In that sense, automated dental radiograph analysis for animals is not just about detection. It can also support better records, better handoffs, and better continuity of care.
What AI for Veterinary Dental Radiograph Interpretation actually does

At a practical level, AI for Veterinary Dental Radiograph Interpretation usually combines computer vision with machine learning. The system is trained on many labeled dental images so it can learn patterns associated with normal anatomy and common abnormalities.
When a new image is uploaded, the software analyzes visual features, compares them with what it has learned, and produces outputs such as flagged regions, likely findings, annotations, confidence indicators, or structured reports for clinician review.
That sounds simple, but several steps are happening behind the scenes. The image may be standardized, checked for orientation, sorted by tooth or quadrant, and then processed through models that look for specific changes. Some systems focus on classification, such as whether disease is likely present.
Others aim for localization, showing the exact area of concern. More advanced veterinary dental imaging AI may provide tooth-by-tooth summaries that help the team move more quickly from image review to charting and treatment planning.
The crucial point is that AI does not “understand” the patient the way a clinician does. It does not know the pet’s pain level, anesthesia history, periodontal probing results, or whether a lesion fits the physical exam. It sees patterns in image data. That makes it powerful for pattern recognition, but incomplete for final decision-making.
The best way to think about artificial intelligence in veterinary imaging is as a second set of digital eyes with narrow strengths. It does not get tired. It can apply the same screening logic repeatedly.
It may notice subtle image patterns that are easy to miss on a rushed review. But it can also be confused by unusual anatomy, poor positioning, motion blur, severe overlap, artifacts, or disease presentations that were not well represented in training data.
That is why responsible use depends on the “human-in-the-loop” model. The software reviews first or alongside the clinician, highlights what it considers important, and the veterinarian makes the final call. Professional discussions around AI in veterinary care increasingly emphasize transparency, safety, privacy, and accountability rather than blind automation.
How machine learning learns from labeled veterinary dental images
Machine learning for veterinary dentistry depends on training data. Experts label images with known findings, such as bone loss, resorptive lesions, retained roots, widened periodontal ligament space, or periapical disease. The model uses those labeled examples to learn which combinations of shapes, edges, densities, and spatial relationships often go with those findings.
Over time, the system becomes better at recognizing patterns that recur across large datasets. But that learning process creates a major practical limitation: the tool becomes only as strong as the data behind it.
If the training set overrepresents clean images from certain sensors, common breeds, or advanced disease while underrepresenting subtle disease, unusual skull types, or technically imperfect films, the real-world performance can drift.
That is one reason practices should ask difficult questions about validation before relying heavily on AI-assisted veterinary radiology.
Was the tool trained on both canine and feline studies? Did it include general-practice image quality, or mainly ideal specialist-quality radiographs? Were findings verified by boarded experts? Has performance been checked across different image acquisition systems? These are not technical details for software people only. They go directly to whether the output is clinically trustworthy.
What the output usually looks like in practice
Most dental radiograph software for veterinarians does not just say “normal” or “abnormal.” It usually produces something more usable: annotated images, tooth-level flags, heatmap-style highlights, structured findings, or a preliminary summary that the clinician can accept, edit, or reject.
Some tools may also help organize images by mouth segment or create a more standardized case review layout.
This matters because workflow value often comes from presentation, not only detection. A tool that identifies likely animal dental pathology detection targets but displays them poorly may slow the team down. A tool with slightly lower technical sophistication but excellent workflow design may save more time and improve review quality in actual practice.
The strongest systems help the veterinarian answer three useful questions quickly: Which teeth need close attention? What type of abnormality is being suggested? What should I verify on my own before I act?
When software supports those steps well, AI veterinary dental radiograph interpretation becomes easier to integrate into real clinic routines rather than feeling like one more screen to click through.
Common dental findings AI may help identify
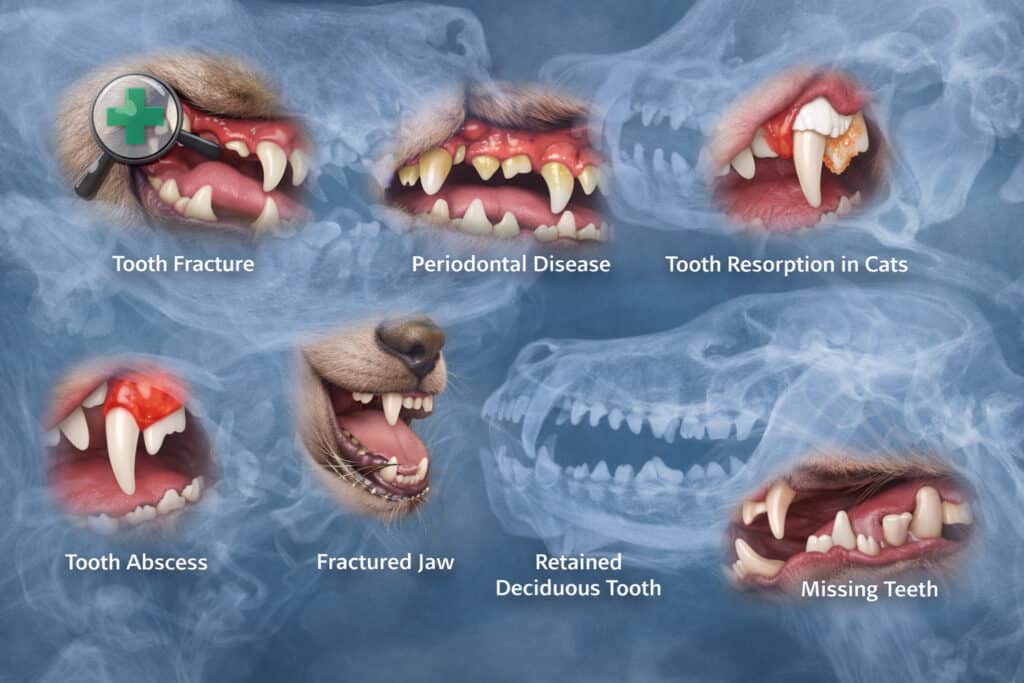
AI in veterinary dentistry is most useful when it is aimed at findings that have recognizable image patterns and real treatment implications. That includes several common dental and oral changes that clinicians already assess routinely on full-mouth radiographs.
The goal is not for the software to invent new diagnoses, but to make important abnormalities easier to detect and review.
Periodontal disease is one major area. AI may help flag horizontal or vertical bone loss, furcation involvement, and changes around tooth support structures that affect prognosis and extraction planning.
Because periodontal disease can involve many teeth in the same patient, a tool that helps standardize tooth-by-tooth review can be genuinely useful, especially in busy general practice settings.
Endodontic and apical changes are another promising category. The software may highlight widened periodontal ligament space, periapical lucency, root abnormalities, or suspicious fracture-related changes.
In some cases, it may support quicker identification of teeth that need closer review for pulp exposure or chronic apical disease. That does not mean the software decides treatment, but it can help the team avoid missing teeth that deserve a second look.
Tooth resorption, retained roots, missing teeth that are not actually absent, and root remnants after prior extractions are also logical targets for automated dental radiograph analysis for animals.
These findings often matter clinically yet can be easy to miss when the review is rushed. AI may also support recognition of obvious tooth fractures, severe crowding-related disease, and certain bone changes associated with advanced oral pathology.
Even so, the phrase “may help identify” is important. Veterinary dental imaging AI should be understood as decision support, not decision authority. It can raise a hand. It cannot replace confirmation.
Periodontal bone loss, furcation change, and supporting structures
Periodontal disease is among the most common and clinically important uses for veterinary dental X-ray interpretation because surface calculus alone does not tell the full story. The real question is what is happening to the supporting tissues around each tooth.
Radiographs help reveal horizontal bone loss, vertical defects, furcation exposure, and other changes that shape treatment decisions and long-term prognosis.
This is where AI veterinary imaging diagnostics may offer real workflow support. A model trained to assess supporting structures can guide attention toward teeth with suspicious bone loss patterns or regions where anatomy suggests more advanced periodontal destruction than the crown appearance alone would imply. In practices that perform many dental procedures, that kind of flagging can make review more systematic.
Still, caution is necessary. Periodontal interpretation is especially sensitive to image angle, exposure, and overlap. Mild changes can be exaggerated or obscured depending on projection. Gingival inflammation, pocket depth, mobility, and probing findings remain essential.
A flagged furcation or bone defect is not a final diagnosis until it fits the complete oral exam. Used properly, AI can help make periodontal review more consistent, but it should never be allowed to outrank what the clinician sees in the patient and on the full study.
Tooth resorption, fractures, retained roots, and apical disease
Another high-value area for AI in veterinary dentistry is the detection of structural tooth disease that may otherwise be subtle or scattered across the mouth. Tooth resorption can be difficult to catch early, especially when crown changes are mild but the root or surrounding bone tells the real story.
Root remnants, retained roots after prior procedures, chronic apical change, and certain fracture-related findings can also be easy to miss if the team is working quickly.
Veterinary dental imaging AI may help by identifying irregular root contours, radiolucent or radiopaque change, loss of normal structure, or suspicious apical regions that deserve targeted review.
For less experienced readers, this can act as a helpful educational prompt. For experienced readers, it can function as a checklist aid, reducing the chance that a single important tooth is overlooked in a large case.
But these categories also show why human oversight remains non-negotiable. Tooth resorption patterns can vary. Superimposition can mimic disease. Prior extractions can create confusing anatomy.
Fracture interpretation may depend on the crown exam, mobility, pain, or case history. In other words, AI-assisted veterinary radiology is strongest when it helps direct attention, not when it is treated as the final voice on structural disease.
The real benefits of AI in veterinary dental imaging

The strongest case for AI for Veterinary Dental Radiograph Interpretation is not that it makes dentistry automatic. It is that it can support better clinical workflow in several practical ways at once.
When implemented well, it can reduce review friction, improve consistency, strengthen documentation, and help teams learn. Those are meaningful benefits in both high-volume general practice and specialty settings.
Speed is the most obvious advantage. Dental procedures often involve many images, a patient under anesthesia, and a treatment plan that may change based on radiographic findings.
If AI veterinary dental radiograph interpretation helps the clinician find likely problem areas faster, the team can move more efficiently from imaging to decision-making. Faster does not mean rushed. It means more of the available time goes into verification, treatment, and communication instead of hunting for the same information repeatedly.
Consistency is just as important. A structured AI review can help make sure every tooth is evaluated, even when the day is busy or multiple team members share case responsibilities.
That reduces variability and can improve the reliability of veterinary oral health diagnostics across doctors, shifts, or locations. In multi-doctor practices, it can also help align expectations around what gets documented and communicated.
There is also a training benefit. Team members who are still building skill in veterinary dental X-ray interpretation can use AI output as a teaching aid. When a flagged region is reviewed alongside anatomy, charting, and clinical findings, it creates feedback that can strengthen learning over time. That does not replace mentorship, but it can reinforce it.
AI may also help with case review assistance, documentation, and client communication. Annotated images and structured summaries can make it easier to explain why a tooth is being monitored, extracted, or referred.
Some practices may find that AI-supported reports improve record quality and make handoffs between team members more efficient. In the broader picture, that contributes to veterinary dental workflow optimization rather than just image analysis.
Speed, triage support, and diagnostic confidence
In real clinics, the value of speed is tied to decision flow. The dentist or veterinarian still needs to confirm findings, but AI can shorten the path to that confirmation by surfacing likely areas of concern early. That can be especially helpful when reviewing full-mouth series, complex oral disease, or cases where multiple extractions are being considered.
Triage support is another practical gain. AI-assisted veterinary radiology can help a general practice identify which cases appear straightforward, which teeth need closer scrutiny, and which cases may deserve referral or specialist input.
That kind of case prioritization can improve scheduling, reduce uncertainty, and help teams use specialist time more effectively when they do seek consultation.
Diagnostic confidence is often discussed carefully, and for good reason. Confidence should come from evidence, not from software polish.
But many clinicians find it useful to have a second review layer, especially when the tool presents findings transparently and encourages verification rather than blind trust. In that setting, AI can increase confidence the right way: by supporting a more thorough review, not by replacing it.
Training support, documentation, and communication with pet owners
AI veterinary dental radiograph interpretation can also improve the parts of dentistry that happen after the image review. For example, a structured report may make charting faster and more complete.
An annotated image can help the team explain pathology to a client who cannot interpret radiographs on sight. That matters because owner understanding often affects consent, treatment acceptance, and follow-through.
For training, the benefit is similar. Less experienced doctors and technicians can compare AI flags with mentor feedback, oral exam findings, and final case outcomes.
Over time, repeated exposure to that loop can strengthen their ability to interpret radiographs independently. In that sense, veterinary dental imaging AI can function like a pattern-recognition coach, provided the team treats it as a teaching aid rather than an answer key.
Documentation matters for another reason too: risk management. Clear records support continuity of care, help defend treatment decisions, and improve internal quality review.
Practices thinking about technology adoption more broadly may also find value in related reading on veterinary practice risk management, especially when evaluating new diagnostic systems.
Practical comparison: where AI helps most and where caution is highest
| Clinical task | How AI may help | Where caution is needed |
| Full-mouth image review | Flags teeth or regions needing closer attention | Can miss subtle lesions or overcall artifacts |
| Periodontal assessment | Supports tooth-by-tooth review for bone loss and furcation concerns | Positioning errors can distort support structures |
| Fracture and apical review | Highlights suspicious root or apical change | Must be correlated with crown exam and history |
| Tooth resorption screening | Points to irregular root or crown-root patterns | Early or atypical lesions may be misclassified |
| Case documentation | Creates structured findings and annotated visuals | Records still need clinician editing and approval |
| Client communication | Makes disease easier to explain visually | Annotations should not be shown as final diagnosis without review |
| Training support | Reinforces systematic reading habits | Overdependence can weaken independent interpretation |
| Referral triage | Helps identify cases that may need specialist review | Referral decisions still require clinician judgment |
Limitations and risks clinicians should never ignore
Every benefit of AI veterinary dental radiograph interpretation comes with a matching limitation. That is not a reason to avoid technology. It is a reason to use it intelligently. The most common problems are not dramatic software failures.
They are quieter issues like bad source images, misread anatomy, underrepresented patient types, edge-case pathology, and human overtrust.
Image quality is the first major issue. If the radiograph is non-diagnostic because of poor angle, motion, overlap, bad exposure, cutoff anatomy, or labeling problems, the software cannot rescue it reliably.
In fact, it may produce confident-looking output on a weak image, which can be more dangerous than no output at all. Correct positioning remains essential in veterinary dental radiography, and no AI layer changes that.
Breed and skull variation also matter. A system trained heavily on one population may behave differently with brachycephalic, dolichocephalic, toy-breed, large-breed, or feline anatomy if those groups were not represented well in training.
That is one reason performance claims should never be accepted in the abstract. Practices need to know how the tool behaves on the kinds of patients they actually see.
False positives and false negatives are inevitable. A false positive can lead to overcalling disease, unnecessary concern, longer procedure time, or inappropriate treatment pressure. A false negative can create false reassurance and potentially missed pain or disease. Human review is the safeguard for both. The tool should improve the clinician’s process, not replace it.
Then there are edge cases. Oral masses, severe destruction, postoperative changes, mixed disease patterns, and unusual anatomy can all challenge machine learning for veterinary dentistry. These are often the very cases where the clinician most needs judgment, context, and sometimes specialist consultation.
Data quality, positioning problems, and artifact-related errors
Automated dental radiograph analysis for animals depends heavily on clean inputs. The model may have been trained on large datasets, but if a new image is stretched, truncated, overlapped, noisy, or poorly exposed, the output can become unreliable fast.
Positioning errors matter because dental findings often depend on subtle relationships between root structure, bone levels, and surrounding tissue boundaries. Distort those relationships, and even a strong model can drift.
Artifacts add another layer of difficulty. Sensor defects, motion blur, processing inconsistencies, foreign objects, prior dental material, and projection artifacts can all create patterns that resemble disease.
A clinician may recognize those issues through experience and context. The model may simply see them as suspicious signals. That increases false-positive risk and may waste time if the software repeatedly highlights the same non-clinical issue.
This is why strong veterinary dental workflow optimization starts with acquisition protocols. If a practice wants useful AI output, it needs consistent image quality standards, naming conventions, positioning checks, and a process for repeating non-diagnostic views. AI is downstream from image quality. It cannot be expected to compensate for weak fundamentals.
False positives, false negatives, and edge cases
A false positive in AI-assisted veterinary radiology may seem less serious than a missed lesion, but it can still have meaningful consequences.
It may push the team toward unnecessary rechecks, overexplaining uncertain findings to owners, or spending time on teeth that are normal while subtler disease sits elsewhere. In a long procedure, even small workflow inefficiencies add up.
False negatives are often the greater worry. When software does not flag a lesion, the clinician may unconsciously lower their guard, especially if they are tired or less experienced with veterinary dental X-ray interpretation. That is why practices should train teams not to use AI as a filter for where to look, but as an additional reason to look carefully.
Edge cases deserve special respect. Unusual anatomy, mixed pathology, advanced destruction, prior oral surgery, and less common conditions may not match what the model learned well.
Those are cases where human expertise and sometimes specialty review remain central. AI for Veterinary Dental Radiograph Interpretation can still be helpful in such cases, but it should be treated as limited assistance, not a dependable authority.
How AI fits into real veterinary dental workflows
The most successful use of AI in veterinary dentistry is usually not dramatic. It becomes part of a predictable workflow. Images are acquired, checked for quality, uploaded or routed automatically, reviewed with AI support, verified by the clinician, and incorporated into charting, treatment planning, and client communication.
When that sequence is smooth, the tool adds value. When it interrupts the team with extra exports, duplicate data entry, or awkward interfaces, it quickly becomes shelfware.
In general practice, the biggest opportunity is often support for consistency. Many clinics perform dentistry regularly but do not have a board-certified dentist on site.
In those environments, AI veterinary dental radiograph interpretation can help standardize image review, guide attention to likely abnormalities, and support treatment discussions before the patient wakes up. It can also help identify which cases are straightforward enough to manage in-house and which might benefit from referral.
In specialty practice or referral settings, the role may shift. The clinician is already highly trained in interpretation, so the software’s value may lie more in workflow acceleration, structured documentation, teaching support, or communication aids.
In academic and training environments, AI may also help demonstrate how a systematic review should be performed, even when the final interpretation still depends on expert oversight.
Integration matters just as much as accuracy. The best systems fit inside existing practice software, PACS, or imaging workflows so that the team is not constantly switching platforms. Articles on cloud-based systems for veterinary practices and workflow technology in veterinary clinics can be helpful for thinking through that broader infrastructure question.
General practice: the “extra set of eyes” model
For many general practices, AI for Veterinary Dental Radiograph Interpretation makes the most sense as an extra set of eyes. The team takes a full-mouth series, reviews the study clinically, then uses AI output to confirm what they saw, surface anything they may have missed, and support documentation.
This model works well because it preserves the veterinarian’s authority while still capturing the software’s strengths in speed and pattern recognition.
A realistic example is a routine dental procedure where multiple teeth show mild to moderate periodontal change, one premolar has a subtle apical concern, and another tooth may have early resorptive change.
Without structured support, the review can feel scattered. With AI, the clinician may get a more organized list of suspect teeth, helping them confirm each one efficiently and make cleaner treatment decisions under anesthesia.
This model also helps when case volume is high or doctor comfort with dentistry varies. The software does not need to be perfect to be useful. It needs to help the team be systematic, reduce oversights, and communicate more clearly.
Specialty, referral, and collaborative review settings
In specialty practice, AI in veterinary dentistry may function less as a detector and more as a workflow assistant. A boarded dentist or radiologist may not need help recognizing classic disease, but they may still benefit from software that speeds image organization, structures reports, or creates annotated visuals for referring veterinarians and clients.
Referral environments also highlight another useful role: collaborative review. AI-generated summaries can support communication between the general practitioner, the specialist, and the nursing team.
When the findings are laid out clearly, it becomes easier to explain which lesions matter most, why specific extractions are recommended, and what follow-up is needed.
That said, specialty settings also expose weaknesses faster. Unusual pathology, advanced disease, prior procedures, and referral-only complexity can strain model performance.
For that reason, specialty teams often make excellent evaluators of whether a tool is truly ready for broader use. If a product does not hold up in expert review, it should not be trusted blindly in general practice.
Ethical, clinical, and legal considerations
As AI veterinary imaging diagnostics become more common, the biggest questions are no longer just technical. They are ethical and operational. Who is accountable for the final interpretation? How transparent should practices be about AI use? How is client data handled?
What happens when the software output conflicts with the clinician’s judgment? These are practical issues that affect trust and risk management, not abstract theory.
Professional discussions in veterinary medicine increasingly emphasize responsible frameworks for AI adoption. Safety, privacy, transparency, and accountability are recurring themes, along with the principle that licensed professionals remain responsible for patient care decisions.
Regulatory guidance has also stressed compliance with applicable practice acts and client-data obligations when AI tools are used in clinical settings.
Clinically, the key principle is simple: AI supports decision-making; it does not replace professional judgment. If a veterinarian follows software output without independent review, the problem is not only diagnostic.
It is also ethical, because the clinician has ceded reasoning to a system that lacks full clinical context. Likewise, if a practice uses AI but hides that fact in ways that would matter to client trust or record accuracy, that can create avoidable risk.
Data handling deserves close attention too. Dental images are part of the medical record. Practices should understand where images are stored, how they are transmitted, whether they are used for further model training, and what security protections apply. Technology convenience should never come at the cost of sloppy information governance.
Transparency, accountability, and informed use
Transparency does not necessarily mean overwhelming clients with technical detail. It means the practice is honest about how it uses diagnostic tools and clear that the veterinarian remains the decision-maker.
If AI helps review dental radiographs, many practices will find it wise to describe that internally as clinical decision support rather than automated diagnosis.
Accountability should be unmistakable. The final interpretation belongs to the veterinarian or specialist reviewing the case. That person should be able to explain what the software flagged, what they agreed with, what they rejected, and why the treatment plan makes sense based on the whole patient. If the record simply parrots AI output without clinician review, that is a weak practice standard.
This is also where documentation matters. Good records should show that radiographs were reviewed, clinically correlated, and incorporated into the final plan. AI can assist with that workflow, but the record should still reflect human oversight.
Responsible frameworks in veterinary medicine increasingly point in this direction because it protects patients, clients, and the clinical team.
Data privacy, compliance, and record quality
From a workflow perspective, privacy and compliance are easy to underestimate because they are less visible than image annotations.
Yet they are essential. Dental images, case notes, and reports may move across local machines, cloud systems, and vendor platforms. Practices need to know where that data goes, who can access it, how long it is stored, and how it is protected.
Record quality matters for legal reasons as well as clinical ones. If AI output is incorporated into a report, it should be reviewed, edited when needed, and saved in a way that makes the final clinical interpretation clear.
Audit trails, user permissions, and secure access become more important as more tools are layered into the imaging workflow. For many practices, those questions intersect with broader infrastructure choices around cloud software, imaging archives, and workflow systems.
What to look for when evaluating an AI dental imaging tool
Practices considering AI for Veterinary Dental Radiograph Interpretation should evaluate it like any other clinical tool: by usefulness, reliability, fit, and risk. Marketing claims alone are not enough. A good evaluation process asks how the system performs, how it integrates, and how it behaves when conditions are less than ideal.
Start with validation. Ask what species the tool covers, what findings it is designed to detect, who labeled the training data, and how real-world performance was measured.
Was it tested on both common and difficult cases? Was general-practice image quality included? Does the vendor provide information about false positives, false negatives, and known weak spots? A tool that cannot discuss its limitations openly is not ready for responsible clinical use.
Next, look at workflow integration. Does it connect to the imaging system the practice already uses? Does it support fast review during procedures? Can findings be edited easily? Does it create useful reports without duplicating work? Veterinary dental workflow optimization depends as much on usability as on algorithm quality.
Usability for clinicians matters too. The output should be understandable at a glance and detailed enough for review. Teeth should be labeled clearly. Flags should be traceable to specific image regions. Reports should help, not clutter. The software should also make it easy to disagree with the AI, because clinicians will need to do that.
Support and training are another major factor. A strong tool comes with onboarding, feedback channels, and updates that respond to clinical reality. Practices should not assume that implementation ends when the contract is signed. Like any medical technology, AI adoption works best when the team knows exactly how the tool should and should not be used.
A practical checklist for comparing AI veterinary dental solutions
When a practice compares options, it helps to use a structured checklist rather than relying on demos alone. Here are useful questions to ask:
- What species and dental conditions are covered?
- Is the tool designed for screening, decision support, reporting, or all three?
- How was the model validated, and by whom?
- What does the vendor disclose about false positives and false negatives?
- Can clinicians edit, reject, or annotate AI findings easily?
- Does the tool integrate with existing imaging and record systems?
- How long does analysis take during a live dental workflow?
- How are images stored, secured, and audited?
- Is the output understandable to both clinicians and clients?
- What training is provided for doctors and technicians?
- What happens during downtime or connectivity issues?
- How does the vendor handle updates and post-launch monitoring?
A practice that answers these questions carefully is far more likely to select a tool that genuinely improves AI veterinary imaging diagnostics instead of complicating them.
Best practices for combining AI output with clinical judgment
The safest and most effective way to use AI for Veterinary Dental Radiograph Interpretation is to combine it with a structured clinical review process. That means the oral exam, charting, periodontal probing, image quality check, radiographic interpretation, and treatment decision all stay connected. AI becomes one component of that process, not a shortcut around it.
A strong workflow usually follows a sequence. First, obtain diagnostic images. Second, confirm the images are correctly oriented and complete enough to interpret. Third, review the study independently or alongside AI output.
Fourth, compare flagged findings with the physical exam and dental chart. Fifth, document the final clinician interpretation and treatment plan. Sixth, use the images and summary to communicate clearly with the pet owner.
This sequence matters because it prevents a common mistake: letting software output shape the entire reading before the clinician has looked carefully.
Many practices find it smarter to review the case first, then use AI as a confirmation and gap-check step. Others prefer a side-by-side review. Either can work, as long as the veterinarian remains active and skeptical in the process.
It is also wise to build escalation rules. For example, if AI and clinician agree, the case proceeds normally. If the AI flags something the clinician did not initially see, that tooth gets a second focused review.
If the clinician suspects significant disease that AI does not flag, the clinician’s concern takes priority. If the case is unusual or complex, specialty input may be sought regardless of what the software says.
A realistic workflow example from image capture to treatment plan
Imagine a middle-aged dog scheduled for a dental procedure. The technician acquires full-mouth radiographs after cleaning and charting. One maxillary tooth appears mildly abnormal on quick visual review, but nothing looks dramatic at first glance.
The images are uploaded into a veterinary dental imaging AI platform that flags several additional teeth for periodontal bone loss, one possible retained root, and one suspicious apical area.
The veterinarian then reviews each flagged region with the full study open. Two of the AI flags are confirmed as clinically important. One flagged “retained root” turns out to be normal overlapping anatomy on a nonideal view, prompting a repeat image.
Another unflagged tooth shows a subtle issue during the veterinarian’s own review and is added to the treatment plan despite the software’s silence.
The final treatment plan is based on the veterinarian’s interpretation, not the software’s list. But the AI still added value. It helped structure the review, surfaced one finding that might have been revisited later, prompted a repeat image on a questionable area, and created annotated visuals that made client communication easier after the procedure. That is a realistic, useful model for AI-assisted veterinary radiology.
When to involve a specialist or seek another review
AI should not reduce referral quality. In fact, used well, it can improve it. Cases with extensive periodontal destruction, severe tooth resorption, jaw pathology, oral masses, unusual root anatomy, complicated fractures, or unclear postoperative findings may still need specialist input regardless of what the software suggests.
A good rule is this: when the clinical stakes are high, the anatomy is unusual, or the treatment could change substantially based on interpretation, seek the level of expertise the case deserves.
AI in veterinary dentistry can help identify those moments, but it should not replace them. In many practices, the best role for AI is helping the team recognize when they are comfortable proceeding and when they are better served by collaboration.
Frequently Asked Questions
Is AI for Veterinary Dental Radiograph Interpretation accurate enough to rely on by itself?
No. AI can be very helpful, but it should not be used as the sole basis for diagnosis or treatment decisions. Veterinary dental radiograph interpretation still requires a licensed clinician to review the full image set, the oral exam, probing findings, patient history, and the complete treatment context. AI works best as decision support, not as a replacement for professional judgment.
Can AI detect every dental problem on a veterinary radiograph?
No tool can detect every problem. AI may help identify common findings such as periodontal bone loss, apical changes, retained roots, fractures, or tooth resorption, but it can also miss subtle, atypical, or poorly imaged disease. It may also flag normal anatomy or artifacts as suspicious, which is why human oversight remains essential.
Is AI more useful in general practice or specialty veterinary dentistry?
It can be useful in both settings, but for different reasons. In general practice, AI often helps as an extra set of eyes and a consistency tool during case review. In specialty settings, it may be more valuable for workflow support, faster reporting, teaching, and case communication. Its usefulness depends on how well it fits the clinic’s workflow and how it supports, rather than replaces, clinical expertise.
Does AI reduce the need for training in veterinary dental X-ray interpretation?
No. Strong training is still necessary. AI is most helpful when the veterinary team already understands anatomy, image quality, positioning, and common dental pathology. Without that foundation, there is a greater risk of overtrusting the software or misreading its suggestions. AI can support learning, but it does not remove the need for education and clinical experience.
What should a veterinary practice look for before choosing dental radiograph software with AI features?
A practice should look at validation standards, supported species, the types of conditions the software is designed to detect, how it handles poor-quality images, and how easily it fits into the existing workflow. It is also important to review data security, reporting tools, ease of editing or rejecting AI findings, and the level of training and support provided by the software vendor.
Can AI help with client communication after a veterinary dental procedure?
Yes. AI-supported annotations and structured summaries can make radiographic findings easier to explain to pet owners. This can help clients better understand why a tooth was extracted, why a lesion matters, or why follow-up care is needed. The key is that any visuals or summaries should be reviewed and confirmed by the veterinarian before they are shared.
Conclusion
The most useful way to view AI for Veterinary Dental Radiograph Interpretation is as a support tool for better care, not as a replacement for clinical expertise.
Veterinary dental radiographs remain essential because so much oral disease is hidden below the gumline, and careful interpretation is central to pain relief, treatment planning, and long-term oral health. AI can help make that interpretation faster, more consistent, and easier to document when it is built into a thoughtful workflow.
Its strengths are practical: pattern recognition, structured review, case organization, training support, documentation help, and communication value.
Its limits are equally practical: weak images, unusual anatomy, breed variation, artifacts, edge cases, and the unavoidable reality of false positives and false negatives. That is why the right message for any practice considering veterinary dental imaging AI is not “trust the software.” It is “use the software well.”
In real clinics, the best results come when AI veterinary dental radiograph interpretation is paired with high-quality image acquisition, a complete oral exam, tooth-by-tooth review, strong documentation, and a veterinarian who stays fully accountable for the final interpretation.
Used that way, AI in veterinary dentistry can improve workflow and support better decisions without diluting professional judgment. And that is exactly where it belongs: inside the clinical process, serving it.